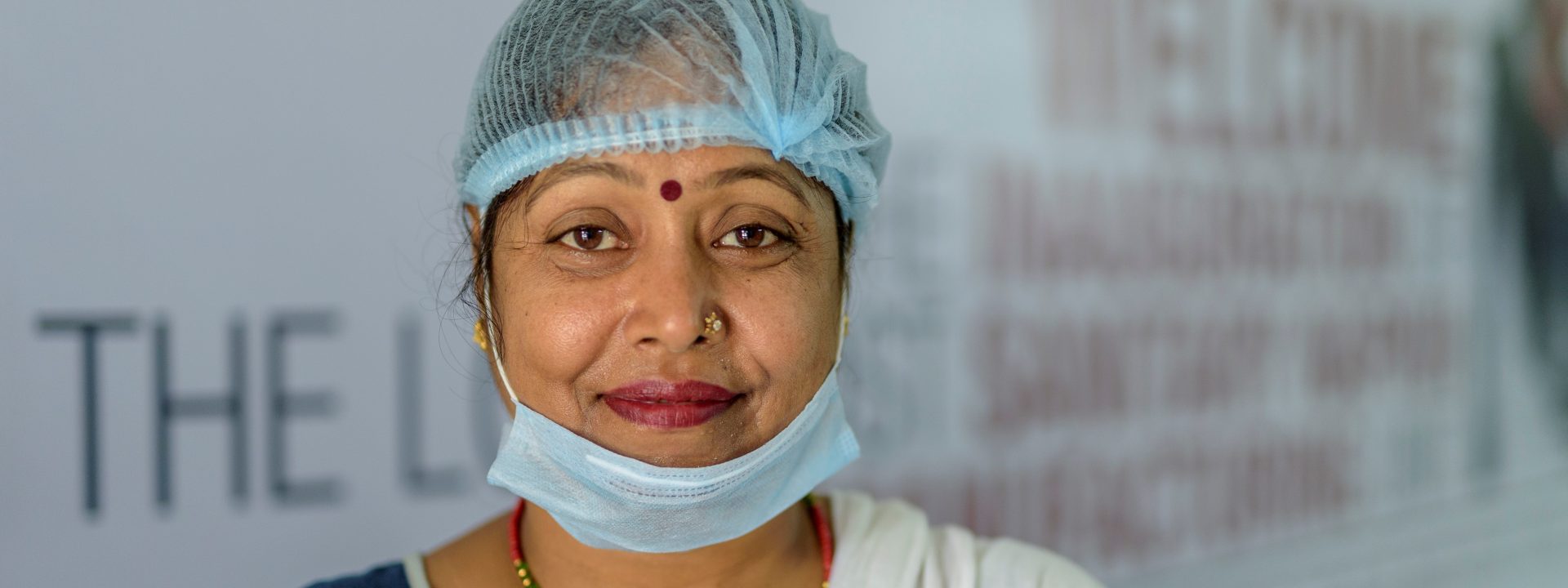
COVID-19 now threatens a health system that has proved powerless to cover the 1.3 billion inhabitants. © Vicente Ferrer Foundation
On April 20th, according to the Dashboard by the Center for Systems Science and Engineering (CSSE) of the Johns Hopkins University, in India there were 17,615 cases of COVID-19 and 559 deaths due to this virus; although these figures are not very relevant due to the lack of diagnostic tests. This is a problem that has occurred in many countries and has been more evident in India: at that time, according to the Indian Council of Medical Research (ICMR), the tests performed were no more than 10 per one million inhabitants, one of the lowest rates in the world. The Government has requested 700,000 diagnostic kits for the areas with the highest risk of infection, the greatest concern being rural areas which, since the outbreak of the pandemic, have received and uncontrolled flow of migrants from cities.
The inverted migration process

Many of inhabitants who are now returning are those who fled rural poverty and ended up crowded into slums without the minimum conditions for a dignified life. © Carlos Garriga/ We Are Water Foundation
India is experiencing a paradox similar to that of many developing countries, whose economic emergence has led to the depopulation of agricultural areas in favor of cities. These countries are now experiencing the opposite phenomenon: many of those who are now returning are those who fled rural poverty and ended up crowded into slums without the minimum conditions for a dignified life. Among them, for example, are the descendants of those who, because of the terrible drought of 1984 – 1986, were ruined and sold off their land in debt. Now, the confinement has drastically stopped the activities of small self-employed workers, such as street vendors, artisans and public servants, including the scavengers, the garbage collectors in the landfills, who have seen their already precarious way of life disappear from one day to the next. Many have begun to return to the regions where they have relatives, most of whom are poor or on the verge of poverty.
The massive overcrowding of migrants on trains meant that there was a clear risk of the disease spreading to the agricultural areas, which have the worst medical coverage in the country and where more than 60% (750 million) of its inhabitants live. Many travelers were trapped on their journey and those who arrived joined the farmers who, after the dry season and waiting for the start of the monsoon, (May-June) already had their food security and access to water compromised. Others, faced with the cancellation of train and bus travel, have begun their diaspora to towns and villages on foot, contravening the confinement and increasing the risk of infection.
The coronavirus ravages a country that every two or three years suffers from lacerating epidemics such as diarrhea, which annually kills more than 10,000 children. Diarrhea, malaria and dengue fever could be fought effectively through good hygiene, the consumption of safe water and the use of adequate sanitation. Although child and maternal mortality have decreased in recent years, deaths from curable medical conditions are a constant in India and keep the country from achieving the Sustainable Development Goals (SDGs) by 2030.
Modicare on the ropes

In Anantapur district, the We Are Water Foundation collaborates in projects that provide access to water and sanitation with the Vicente Ferrer Foundation.
The lack of access to water and especially to sanitation are the main obstacles. In 2015, the World Health Organization (WHO) estimated that only 39% of the inhabitants of rural India have access to sanitation facilities, and that 564 of the 946 million people in the world who defecate in the open live in India, 61% of them in rural areas. This unhealthy practice mainly harms women in the poorest areas, such as the villages of the Anantapur district, where the We Are Water Foundation collaborates in projects that provide access to water and sanitation with the Vicente Ferrer Foundation. There it is common for women to have to walk up to one kilometer in the dark, in the early hours of the morning, in order to reach open spaces where to defecate.
The Government has set out to address this endemic lack of sanitation with the Swachh Bharat (Clean India) mission, which aims to stop open defecation and promote sanitation throughout the country. The program, which is now entering its second stage, is linked to the Flagship Health Protection Scheme (PMJAY, in Hindi), launched in 2018, which aims to provide health coverage to 40% of the population (500 million people) and reach 100 million of the most vulnerable households. Nicknamed Modicare, in reference to the name of the Prime Minister (Narendra Modi), the plan aims to increase investment in the health sector by 15% and was announced by the government as the world’s largest public health program.

Collaborators of the Vicente Ferrer Foundation deliver food © Vicente Ferrer Foundation
The COVID-19 puts unexpected and alarming pressure on Modicare. According to the WHO, at the time the emergency broke out early March, the country had one doctor for every 10,000 inhabitants, one public hospital for every 55,000 and one isolation bed for every 84,000. With a per capita investment of $267 in health, the shortcomings of Indian public health have increased the preponderance of private health care: 63% of health care spending is now borne by families. According to the group for the defense of universal healthcare, Jan Arogya Abhiyan, a private medical consultation costs an average of 11.5 euros, leaving millions of Indian people, who cannot afford to pay this, without any health coverage.
With a deficit of 600,000 doctors and two million nurses, the Government assures it will double this expenditure in five years, but the needs of the pandemic are immediate. This pressure especially shifts to rural areas where 70% of health resources are lacking. There, one of the hospitals of the Vicente Ferrer Foundation, in Bathalapalli, has been declared by the administration of the state of Andhra Pradesh as a reference center for patients with COVID-19. The Government will strengthen the medical and health staff, both for the hospital and the laboratory, in order to test the patients and process them in the same center. Since the beginning of the pandemic, the hospital has been manufacturing disinfectant gels, and women with disabilities have been making masks. An isolation ward is being set up in the hospital and the Foundation has offered other infrastructure, now empty as a result of the confinement, such as schools or offices for health use.
Many things need to change

One of the hospitals of the Vicente Ferrer Foundation, in Bathalapalli, has been declared by the administration of the state of Andhra Pradesh as a reference center for patients with COVID-19. © Vicente Ferrer Foundation
Shortly after the confinement was announced, the government allocated more than 20 billion euros to aid the most needy and an insurance scheme of more than 60,500 euros for each health professional. The plan, which is ambitious and necessary, has its main obstacles in the corruption and caste structure of Indian society, which must be eradicated. The Indian press has denounced on several occasions the fraudulent diversion of much of the aid provided for in the Modicare and the health system, which as in other sectors tends to benefit the upper classes and castes to the detriment of the lower ones.
In this context, communication also fails. The essential information on the nature of the disease and the dynamics of contagion has to reach social strata in which the practice of open defecation is still common, and female intimate hygiene is a taboo. This reality shows the seriousness of the problem, and the extraordinary humanitarian challenge faced by the world’s most populous democracy.